Programmed cell death protein 1
Programmed cell death protein 1 (PD-1), (CD279 cluster of differentiation 279). PD-1 is a protein encoded in humans by the PDCD1 gene.[5][6] PD-1 is a cell surface receptor on T cells and B cells that has a role in regulating the immune system's response to the cells of the human body by down-regulating the immune system and promoting self-tolerance by suppressing T cell inflammatory activity. This prevents autoimmune diseases, but it can also prevent the immune system from killing cancer cells.[7]
PD-1 is an immune checkpoint and guards against autoimmunity through two mechanisms. First, it promotes apoptosis (programmed cell death) of antigen-specific T-cells in lymph nodes. Second, it reduces apoptosis in regulatory T cells (anti-inflammatory, suppressive T cells).[8][9]
PD-1 inhibitors, a new class of drugs that block PD-1, activate the immune system to attack tumors and are used to treat certain types of cancer.[7][10]
PD-1 is a cell surface receptor that belongs to the immunoglobulin superfamily and is expressed on T cells and pro-B cells.[6] PD-1 binds two ligands, PD-L1 and PD-L2.
Discovery
[edit]In a screen for genes involved in apoptosis, Yasumasa Ishida, Tasuku Honjo and colleagues at Kyoto University in 1992 discovered and named PD-1.[11][12] In 1999, the same group demonstrated that mice where PD-1 was knocked down were prone to autoimmune disease and hence concluded that PD-1 was a negative regulator of immune responses.[12]
Structure
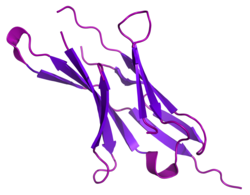
[edit]PD-1 is a type I membrane protein of 288 amino acids. PD-1 is a member of the extended CD28/CTLA-4 family of T cell regulators.[11] The protein's structure includes an extracellular IgV domain followed by a transmembrane region and an intracellular tail. The intracellular tail contains two phosphorylation sites located in an immunoreceptor tyrosine-based inhibitory motif and an immunoreceptor tyrosine-based switch motif, which suggests that PD-1 negatively regulates T-cell receptor TCR signals.[11][13] This is consistent with binding of SHP-1 and SHP-2 phosphatases to the cytoplasmic tail of PD-1 upon ligand binding. In addition, PD-1 ligation up-regulates E3-ubiquitin ligases CBL-b and c-CBL that trigger T cell receptor down-modulation.[14] PD-1 is expressed on the surface of activated T cells, B cells, and macrophages,[15] suggesting that compared to CTLA-4, PD-1 more broadly negatively regulates immune responses.
Ligands
[edit]PD-1 has two ligands, PD-L1 and PD-L2, which are members of the B7 family.[16][17] PD-L1 protein is upregulated on macrophages and dendritic cells (DC) in response to LPS and GM-CSF treatment, and on T cells and B cells upon TCR and B cell receptor signaling, whereas in resting mice, PD-L1 mRNA can be detected in the heart, lung, thymus, spleen, and kidney.[16][18] PD-L1 is expressed on almost all murine tumor cell lines, including PA1 myeloma, P815 mastocytoma, and B16 melanoma upon treatment with IFN-γ.[19][20] PD-L2 expression is more restricted and is expressed mainly by DCs and a few tumor lines.[17]
Function
[edit]Several lines of evidence suggest that PD-1 and its ligands negatively regulate immune responses. PD-1 knockout mice have been shown to develop lupus-like glomerulonephritis and dilated cardiomyopathy on the C57BL/6 and BALB/c backgrounds, respectively.[21][22] In vitro, treatment of anti-CD3 stimulated T cells with PD-L1-Ig results in reduced T cell proliferation and IFN-γ secretion.[16] IFN-γ is a key pro-inflammatory cytokine that promotes T cell inflammatory activity. Reduced T cell proliferation was also correlated with attenuated IL-2 secretion and together, these data suggest that PD-1 negatively regulates T cell responses.[23]
Experiments using PD-L1 transfected DCs and PD-1 expressing transgenic (Tg) CD4+ and CD8+ T cells suggest that CD8+ T cells are more susceptible to inhibition by PD-L1, although this could be dependent on the strength of TCR signaling. Consistent with a role in negatively regulating CD8+ T cell responses, using an LCMV viral vector model of chronic infection, Rafi Ahmed's group showed that the PD-1-PD-L1 interaction inhibits activation, expansion and acquisition of effector functions of virus specific CD8+ T cells, which can be reversed by blocking the PD-1-PD-L1 interaction.[24]
Expression of PD-L1 on tumor cells inhibits anti-tumor activity through engagement of PD-1 on effector T cells.[19][20] Expression of PD-L1 on tumors is correlated with reduced survival in esophageal, pancreatic and other types of cancers, highlighting this pathway as a target for immunotherapy.[7][25] Triggering PD-1, expressed on monocytes and up-regulated upon monocytes activation, by its ligand PD-L1 induces IL-10 production which inhibits CD4 T-cell function.[26]
In mice, expression of this gene is induced in the thymus when anti-CD3 antibodies are injected and large numbers of thymocytes undergo apoptosis. Mice deficient for this gene bred on a BALB/c background developed dilated cardiomyopathy and died from congestive heart failure. These studies suggest that this gene product may also be important in T cell function and contribute to the prevention of autoimmune diseases.[6]
Overexpression of PD1 on CD8+ T cells is one of the indicators of T-cell exhaustion (e.g. in chronic infection or cancer).[7][27]
Clinical significance
[edit]Cancer
[edit]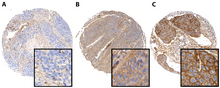
PD-L1, the ligand for PD1, is highly expressed in several cancers and hence the role of PD1 in cancer immune evasion is well established.[29][30][7] Monoclonal antibodies targeting PD-1 that boost the immune system are being developed for the treatment of cancer.[7][31] Many tumor cells express PD-L1, an immunosuppressive PD-1 ligand; inhibition of the interaction between PD-1 and PD-L1 can enhance T-cell responses in vitro and mediate preclinical antitumor activity. This is known as immune checkpoint blockade.
Combination therapy using both anti-PD1 along with anti-CTLA4 therapeutics have emerged as important tumor treatments within the field of checkpoint inhibition.
A combination of PD1 and CTLA4 antibodies has been shown to be more effective than either antibody alone in the treatment of a variety of cancers. The effects of the two antibodies do not appear to be redundant.[7][32][33][34] Anti-CTLA4 treatment leads to an enhanced antigen specific T cell dependent immune reaction while anti-PD-1 appears to reactivate CD8+ T cells ability to lyse cancer cells.[7][35][36]
In clinical trials, combination therapy has been shown to be effective in reducing tumor size in patients that are unresponsive to single co-inhibitory blockade, despite increasing levels of toxicity due to anti-CTLA4 treatment.[37] A combination of PD1 and CTLA4 induced up to a ten-fold higher number of CD8+ T cells that are actively infiltrating the tumor tissue.[35] The authors hypothesized that the higher levels of CD8+ T cell infiltration was due to anti-CTLA-4 inhibited the conversion of CD4 T cells to T regulator cells and further reduced T regulatory suppression with anti-PD-1. This combination promoted a more robust inflammatory response to the tumor that reduced the size of the cancer. Most recently, the FDA has approved a combination therapy with both anti-CTLA4 (ipilimumab) and anti-PD1 (nivolumab) in October 2015.[38]
The molecular factors and receptors necessary making a tumor receptive to anti-PD1 treatment remains unknown. PD-L1 expression on the surface on cancer cells plays a significant role. PD-L1 positive tumors were twice as likely to respond to combination treatment.[38][37] However patients with PD-L1 negative tumors also have limited response to anti-PD1, demonstrating that PD-L1 expression is not an absolute determinant of the effectiveness of therapy.[38]
Higher mutational burden in the tumor is correlated with a greater effect of the anti-PD-1 treatment. In clinical trials, patients who benefited from anti-PD1 treatment had cancers, such as melanoma, bladder cancer, and gastric cancer, that had a median higher average number of mutations than the patients who did not respond to the therapy. However, the correlation between higher tumor burden and the clinical effectiveness of PD-1 immune blockade is still uncertain.[38]
The 2018 Nobel Prize for Medicine was awarded to James P Allison and Tasuku Honjo "for their discovery of cancer therapy by inhibition of negative immune regulation".
Anti-PD-1 therapeutics
[edit]A number of cancer immunotherapy agents that target the PD-1 receptor have been developed.
One such anti-PD-1 antibody drug, nivolumab, (Opdivo - Bristol Myers Squibb), produced complete or partial responses in non-small-cell lung cancer, melanoma, and renal-cell cancer, in a clinical trial with a total of 296 patients.[39] Colon and pancreatic cancer did not have a response. Nivolumab (Opdivo, Bristol-Myers Squibb) was approved in Japan in July 2014 and by the US FDA in December 2014 to treat metastatic melanoma.
Pembrolizumab (Keytruda, MK-3475, Merck), which also targets PD-1 receptors, was approved by the FDA in Sept 2014 to treat metastatic melanoma. Pembrolizumab has been made accessible to advanced melanoma patients in the UK via UK Early Access to Medicines Scheme (EAMS) in March 2015. It is being used in clinical trials in the US for lung cancer, lymphoma, and mesothelioma. It has had measured success, with little side effects.[7] It is up to the manufacturer of the drug to submit application to the FDA for approval for use in these diseases. On October 2, 2015, Pembrolizumab was approved by FDA for advanced (metastatic) non-small cell lung cancer (NSCLC) patients whose disease has progressed after other treatments.[40]
Toripalimab is a humanized IgG4 monoclonal antibody against PD-1 which was approved in China in 2018 and in the United States in 2023.[41][42][43]
Drugs in early stage development targeting PD-1 receptors (checkpoint inhibitors) include pidilizumab (CT-011, Cure Tech) and BMS-936559 (Bristol Myers Squibb). Both atezolizumab (MPDL3280A, Roche) and avelumab (Merck KGaA, Darmstadt, Germany and Pfizer) target the similar PD-L1 receptor.
Animal studies
[edit]HIV
[edit]Drugs targeting PD-1 in combination with other negative immune checkpoint receptors, such as (TIGIT), may augment immune responses and/or facilitate HIV eradication.[44][45] T lymphocytes exhibit elevated expression of PD-1 in cases of chronic HIV infection.[46] Heightened presence of the PD-1 receptors corresponds to exhaustion of the HIV specific CD8+ cytotoxic and CD4+ helper T cell populations that are vital in combating the virus. Immune blockade of PD-1 resulted in restoration of T cell inflammatory phenotype necessary to combat the progression of disease.[46]
Alzheimer's disease
[edit]Blocking of PD-1 leads to a reduction in cerebral amyloid-β plaques and improves cognitive performance in mice.[47] Immune blockade of PD-1 evoked an IFN-γ dependent immune response that recruited monocyte-derived macrophages to the brain that were then capable of clearing the amyloid-β plaques from the tissue. Repeated administrations with anti-PD-1 were found to be necessary to maintain the therapeutic effects of the treatment. Amyloid fibrils are immunosuppressive and this finding has been separately confirmed by examining the effects of the fibrils in neuroinflammatory diseases.[48][49][50] PD-1 counteracts the effects of the fibrils by boosting immune activity and triggering an immune pathway that allows for brain repair.[47]
References
[edit]- ^ a b c ENSG00000276977 GRCh38: Ensembl release 89: ENSG00000188389, ENSG00000276977 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000026285 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ Shinohara T, Taniwaki M, Ishida Y, Kawaichi M, Honjo T (October 1994). "Structure and chromosomal localization of the human PD-1 gene (PDCD1)". Genomics. 23 (3): 704–6. doi:10.1006/geno.1994.1562. PMID 7851902.
- ^ a b c "Entrez Gene: PDCD1 programmed cell death 1".
- ^ a b c d e f g h i Syn NL, Teng MW, Mok TS, Soo RA (December 2017). "De-novo and acquired resistance to immune checkpoint targeting". The Lancet. Oncology. 18 (12): e731–e741. doi:10.1016/s1470-2045(17)30607-1. PMID 29208439.
- ^ Francisco LM, Sage PT, Sharpe AH (July 2010). "The PD-1 pathway in tolerance and autoimmunity". Immunological Reviews. 236: 219–42. doi:10.1111/j.1600-065X.2010.00923.x. PMC 2919275. PMID 20636820.
- ^ Fife BT, Pauken KE (January 2011). "The role of the PD-1 pathway in autoimmunity and peripheral tolerance". Annals of the New York Academy of Sciences. 1217 (1): 45–59. Bibcode:2011NYASA1217...45F. doi:10.1111/j.1749-6632.2010.05919.x. PMID 21276005. S2CID 23843848.
- ^ Loftus P (16 Nov 2014). "New Bristol-Myers Drug Helped Skin-Cancer Patients in Trial Live Longer". Wall Street Journal. Retrieved 24 Nov 2014.
- ^ a b c Ishida Y, Agata Y, Shibahara K, Honjo T (November 1992). "Induced expression of PD-1, a novel member of the immunoglobulin gene superfamily, upon programmed cell death". The EMBO Journal. 11 (11): 3887–95. doi:10.1002/j.1460-2075.1992.tb05481.x. PMC 556898. PMID 1396582.
- ^ a b Bardhan K, Anagnostou T, Boussiotis VA (2016). "The PD1:PD-L1/2 Pathway from Discovery to Clinical Implementation". Frontiers in Immunology. 7: 550. doi:10.3389/fimmu.2016.00550. PMC 5149523. PMID 28018338.
- ^ Blank C, Mackensen A (May 2007). "Contribution of the PD-L1/PD-1 pathway to T-cell exhaustion: an update on implications for chronic infections and tumor evasion". Cancer Immunology, Immunotherapy. 56 (5): 739–45. doi:10.1007/s00262-006-0272-1. PMC 11030209. PMID 17195077. S2CID 11384162.
- ^ Karwacz K, Bricogne C, MacDonald D, Arce F, Bennett CL, Collins M, Escors D (October 2011). "PD-L1 co-stimulation contributes to ligand-induced T cell receptor down-modulation on CD8+ T cells". EMBO Molecular Medicine. 3 (10): 581–92. doi:10.1002/emmm.201100165. PMC 3191120. PMID 21739608.
- ^ Agata Y, Kawasaki A, Nishimura H, Ishida Y, Tsubata T, Yagita H, Honjo T (May 1996). "Expression of the PD-1 antigen on the surface of stimulated mouse T and B lymphocytes". International Immunology. 8 (5): 765–72. doi:10.1093/intimm/8.5.765. PMID 8671665.
- ^ a b c Freeman GJ, Long AJ, Iwai Y, Bourque K, Chernova T, Nishimura H, Fitz LJ, Malenkovich N, Okazaki T, Byrne MC, Horton HF, Fouser L, Carter L, Ling V, Bowman MR, Carreno BM, Collins M, Wood CR, Honjo T (October 2000). "Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation". The Journal of Experimental Medicine. 192 (7): 1027–34. doi:10.1084/jem.192.7.1027. PMC 2193311. PMID 11015443.
- ^ a b Latchman Y, Wood CR, Chernova T, Chaudhary D, Borde M, Chernova I, Iwai Y, Long AJ, Brown JA, Nunes R, Greenfield EA, Bourque K, Boussiotis VA, Carter LL, Carreno BM, Malenkovich N, Nishimura H, Okazaki T, Honjo T, Sharpe AH, Freeman GJ (March 2001). "PD-L2 is a second ligand for PD-1 and inhibits T cell activation". Nature Immunology. 2 (3): 261–8. doi:10.1038/85330. PMID 11224527. S2CID 27659586.
- ^ Yamazaki T, Akiba H, Iwai H, Matsuda H, Aoki M, Tanno Y, Shin T, Tsuchiya H, Pardoll DM, Okumura K, Azuma M, Yagita H (November 2002). "Expression of programmed death 1 ligands by murine T cells and APC". Journal of Immunology. 169 (10): 5538–45. doi:10.4049/jimmunol.169.10.5538. PMID 12421930.
- ^ a b Iwai Y, Ishida M, Tanaka Y, Okazaki T, Honjo T, Minato N (September 2002). "Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade". Proceedings of the National Academy of Sciences of the United States of America. 99 (19): 12293–7. Bibcode:2002PNAS...9912293I. doi:10.1073/pnas.192461099. PMC 129438. PMID 12218188.
- ^ a b Blank C, Brown I, Peterson AC, Spiotto M, Iwai Y, Honjo T, Gajewski TF (February 2004). "PD-L1/B7H-1 inhibits the effector phase of tumor rejection by T cell receptor (TCR) transgenic CD8+ T cells". Cancer Research. 64 (3): 1140–5. doi:10.1158/0008-5472.CAN-03-3259. PMID 14871849.
- ^ Nishimura H, Nose M, Hiai H, Minato N, Honjo T (August 1999). "Development of lupus-like autoimmune diseases by disruption of the PD-1 gene encoding an ITIM motif-carrying immunoreceptor". Immunity. 11 (2): 141–51. doi:10.1016/S1074-7613(00)80089-8. PMID 10485649.
- ^ Nishimura H, Okazaki T, Tanaka Y, Nakatani K, Hara M, Matsumori A, Sasayama S, Mizoguchi A, Hiai H, Minato N, Honjo T (January 2001). "Autoimmune dilated cardiomyopathy in PD-1 receptor-deficient mice". Science. 291 (5502): 319–22. Bibcode:2001Sci...291..319N. doi:10.1126/science.291.5502.319. PMID 11209085.
- ^ Carter L, Fouser LA, Jussif J, Fitz L, Deng B, Wood CR, Collins M, Honjo T, Freeman GJ, Carreno BM (March 2002). "PD-1:PD-L inhibitory pathway affects both CD4(+) and CD8(+) T cells and is overcome by IL-2". European Journal of Immunology. 32 (3): 634–43. doi:10.1002/1521-4141(200203)32:3<634::AID-IMMU634>3.0.CO;2-9. PMID 11857337.
- ^ Barber DL, Wherry EJ, Masopust D, Zhu B, Allison JP, Sharpe AH, Freeman GJ, Ahmed R (February 2006). "Restoring function in exhausted CD8 T cells during chronic viral infection". Nature. 439 (7077): 682–7. Bibcode:2006Natur.439..682B. doi:10.1038/nature04444. PMID 16382236. S2CID 205210800.
- ^ Ohigashi Y, Sho M, Yamada Y, Tsurui Y, Hamada K, Ikeda N, Mizuno T, Yoriki R, Kashizuka H, Yane K, Tsushima F, Otsuki N, Yagita H, Azuma M, Nakajima Y (April 2005). "Clinical significance of programmed death-1 ligand-1 and programmed death-1 ligand-2 expression in human esophageal cancer". Clinical Cancer Research. 11 (8): 2947–53. doi:10.1158/1078-0432.CCR-04-1469. PMID 15837746.
- ^ Said EA, Dupuy FP, Trautmann L, Zhang Y, Shi Y, El-Far M, Hill BJ, Noto A, Ancuta P, Peretz Y, Fonseca SG, Van Grevenynghe J, Boulassel MR, Bruneau J, Shoukry NH, Routy JP, Douek DC, Haddad EK, Sekaly RP (April 2010). "Programmed death-1-induced interleukin-10 production by monocytes impairs CD4+ T cell activation during HIV infection". Nature Medicine. 16 (4): 452–9. doi:10.1038/nm.2106. PMC 4229134. PMID 20208540.
- ^ Pauken KE, Wherry EJ (2015). "Overcoming T cell exhaustion in infection and cancer". Trends in Immunology. 36 (4): 265–76. doi:10.1016/j.it.2015.02.008. PMC 4393798. PMID 25797516.
- ^ Müller T, Braun M, Dietrich D, Aktekin S, Höft S, Kristiansen G, et al. (August 2017). "PD-L1: a novel prognostic biomarker in head and neck squamous cell carcinoma". Oncotarget. 8 (32): 52889–52900. doi:10.18632/oncotarget.17547. PMC 5581079. PMID 28881780.
- "Figure 1 - available via license: Creative Commons Attribution 3.0 Unported" - ^ Wang X, Teng F, Kong L, Yu J (August 2016). "PD-L1 expression in human cancers and its association with clinical outcomes". OncoTargets and Therapy. 9: 5023–39. doi:10.2147/OTT.S105862. PMC 4990391. PMID 27574444.
- ^ Gandini S, Massi D, Mandalà M (April 2016). "PD-L1 expression in cancer patients receiving anti PD-1/PD-L1 antibodies: A systematic review and meta-analysis". Critical Reviews in Oncology/Hematology. 100: 88–98. doi:10.1016/j.critrevonc.2016.02.001. PMID 26895815.
- ^ Weber J (October 2010). "Immune checkpoint proteins: a new therapeutic paradigm for cancer--preclinical background: CTLA-4 and PD-1 blockade". Seminars in Oncology. 37 (5): 430–9. doi:10.1053/j.seminoncol.2010.09.005. PMID 21074057.
- ^ Herbst RS, Soria JC, Kowanetz M, Fine GD, Hamid O, Gordon MS, Sosman JA, McDermott DF, Powderly JD, Gettinger SN, Kohrt HE, Horn L, Lawrence DP, Rost S, Leabman M, Xiao Y, Mokatrin A, Koeppen H, Hegde PS, Mellman I, Chen DS, Hodi FS (November 2014). "Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients". Nature. 515 (7528): 563–7. Bibcode:2014Natur.515..563H. doi:10.1038/nature14011. PMC 4836193. PMID 25428504.
- ^ Snyder A, Makarov V, Merghoub T, Yuan J, Zaretsky JM, Desrichard A, Walsh LA, Postow MA, Wong P, Ho TS, Hollmann TJ, Bruggeman C, Kannan K, Li Y, Elipenahli C, Liu C, Harbison CT, Wang L, Ribas A, Wolchok JD, Chan TA (December 2014). "Genetic basis for clinical response to CTLA-4 blockade in melanoma". The New England Journal of Medicine. 371 (23): 2189–99. doi:10.1056/nejmoa1406498. PMC 4315319. PMID 25409260.
- ^ Buchbinder EI, Desai A (February 2016). "CTLA-4 and PD-1 Pathways: Similarities, Differences, and Implications of Their Inhibition". American Journal of Clinical Oncology. 39 (1): 98–106. doi:10.1097/COC.0000000000000239. PMC 4892769. PMID 26558876.
- ^ a b Curran MA, Montalvo W, Yagita H, Allison JP (March 2010). "PD-1 and CTLA-4 combination blockade expands infiltrating T cells and reduces regulatory T and myeloid cells within B16 melanoma tumors". Proceedings of the National Academy of Sciences of the United States of America. 107 (9): 4275–80. Bibcode:2010PNAS..107.4275C. doi:10.1073/pnas.0915174107. PMC 2840093. PMID 20160101.
- ^ Sliwkowski MX, Mellman I (September 2013). "Antibody therapeutics in cancer". Science. 341 (6151): 1192–8. Bibcode:2013Sci...341.1192S. doi:10.1126/science.1241145. PMID 24031011. S2CID 29830409.
- ^ a b Chen DS, Mellman I (July 2013). "Oncology meets immunology: the cancer-immunity cycle". Immunity. 39 (1): 1–10. doi:10.1016/j.immuni.2013.07.012. PMID 23890059.
- ^ a b c d Topalian SL, Taube JM, Anders RA, Pardoll DM (May 2016). "Mechanism-driven biomarkers to guide immune checkpoint blockade in cancer therapy". Nature Reviews. Cancer. 16 (5): 275–87. doi:10.1038/nrc.2016.36. PMC 5381938. PMID 27079802.
- ^ Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, Powderly JD, Carvajal RD, Sosman JA, Atkins MB, Leming PD, Spigel DR, Antonia SJ, Horn L, Drake CG, Pardoll DM, Chen L, Sharfman WH, Anders RA, Taube JM, McMiller TL, Xu H, Korman AJ, Jure-Kunkel M, Agrawal S, McDonald D, Kollia GD, Gupta A, Wigginton JM, Sznol M (June 2012). "Safety, activity, and immune correlates of anti-PD-1 antibody in cancer". The New England Journal of Medicine. 366 (26): 2443–54. doi:10.1056/NEJMoa1200690. PMC 3544539. PMID 22658127.
- Andrew Pollack (June 1, 2012). "Drug Helps Defense System Fight Cancer". The New York Times.
- ^ "FDA approves Keytruda for advanced non-small cell lung cancer". U.S. Food and Drug Administration (FDA) Press Release. 2 October 2015.
- ^ "Toripalimab - Shanghai Junshi Biosciences - AdisInsight". adisinsight.springer.com. Retrieved 2019-08-25.
- ^ Keam, S.J. (2019). "Toripalimab: First Global Approval". Drugs. 79 (5): 573–578. doi:10.1007/s40265-019-01076-2. PMID 30805896.
- ^ "FDA approves toripalimab-tpzi for nasopharyngeal carcinoma". US Food and Drug Administration. October 27, 2023.
- ^ Porichis F, Kaufmann DE (March 2012). "Role of PD-1 in HIV pathogenesis and as target for therapy". Current HIV/AIDS Reports. 9 (1): 81–90. doi:10.1007/s11904-011-0106-4. PMC 3731769. PMID 22198819.
- ^ Chew GM, Fujita T, Webb GM, Burwitz BJ, Wu HL, Reed JS, Hammond KB, Clayton KL, Ishii N, Abdel-Mohsen M, Liegler T, Mitchell BI, Hecht FM, Ostrowski M, Shikuma CM, Hansen SG, Maurer M, Korman AJ, Deeks SG, Sacha JB, Ndhlovu LC (January 2016). "TIGIT Marks Exhausted T Cells, Correlates with Disease Progression, and Serves as a Target for Immune Restoration in HIV and SIV Infection". PLOS Pathogens. 12 (1): e1005349. doi:10.1371/journal.ppat.1005349. PMC 4704737. PMID 26741490.
- ^ a b Velu V, Shetty RD, Larsson M, Shankar EM (February 2015). "Role of PD-1 co-inhibitory pathway in HIV infection and potential therapeutic options". Retrovirology. 12: 14. doi:10.1186/s12977-015-0144-x. PMC 4340294. PMID 25756928.
- ^ a b Baruch K, Deczkowska A, Rosenzweig N, Tsitsou-Kampeli A, Sharif AM, Matcovitch-Natan O, Kertser A, David E, Amit I, Schwartz M (February 2016). "PD-1 immune checkpoint blockade reduces pathology and improves memory in mouse models of Alzheimer's disease". Nature Medicine. 22 (2): 135–7. doi:10.1038/nm.4022. PMID 26779813. S2CID 20699898.
- ^ Kurnellas MP, Adams CM, Sobel RA, Steinman L, Rothbard JB (April 2013). "Amyloid fibrils composed of hexameric peptides attenuate neuroinflammation". Science Translational Medicine. 5 (179): 179ra42. doi:10.1126/scitranslmed.3005681. PMC 3684024. PMID 23552370.
- ^ Kurnellas MP, Ghosn EE, Schartner JM, Baker J, Rothbard JJ, Negrin RS, Herzenberg LA, Fathman CG, Steinman L, Rothbard JB (December 2015). "Amyloid fibrils activate B-1a lymphocytes to ameliorate inflammatory brain disease". Proceedings of the National Academy of Sciences of the United States of America. 112 (49): 15016–23. Bibcode:2015PNAS..11215016K. doi:10.1073/pnas.1521206112. PMC 4679000. PMID 26621719.
- ^ Kurnellas MP, Schartner JM, Fathman CG, Jagger A, Steinman L, Rothbard JB (August 2014). "Mechanisms of action of therapeutic amyloidogenic hexapeptides in amelioration of inflammatory brain disease". The Journal of Experimental Medicine. 211 (9): 1847–56. doi:10.1084/jem.20140107. PMC 4144739. PMID 25073790.
Further reading
[edit]- Vibhakar R, Juan G, Traganos F, Darzynkiewicz Z, Finger LR (April 1997). "Activation-induced expression of human programmed death-1 gene in T-lymphocytes". Experimental Cell Research. 232 (1): 25–8. doi:10.1006/excr.1997.3493. PMID 9141617.
- Finger LR, Pu J, Wasserman R, Vibhakar R, Louie E, Hardy RR, Burrows PD, Billips LG (September 1997). "The human PD-1 gene: complete cDNA, genomic organization, and developmentally regulated expression in B cell progenitors". Gene. 197 (1–2): 177–87. doi:10.1016/S0378-1119(97)00260-6. PMID 9332365.
- Iwai Y, Okazaki T, Nishimura H, Kawasaki A, Yagita H, Honjo T (October 2002). "Microanatomical localization of PD-1 in human tonsils". Immunology Letters. 83 (3): 215–20. doi:10.1016/S0165-2478(02)00088-3. PMID 12095712.
- Prokunina L, Castillejo-López C, Oberg F, Gunnarsson I, Berg L, Magnusson V, Brookes AJ, Tentler D, Kristjansdóttir H, Gröndal G, Bolstad AI, Svenungsson E, Lundberg I, Sturfelt G, Jönssen A, Truedsson L, Lima G, Alcocer-Varela J, Jonsson R, Gyllensten UB, Harley JB, Alarcón-Segovia D, Steinsson K, Alarcón-Riquelme ME (December 2002). "A regulatory polymorphism in PDCD1 is associated with susceptibility to systemic lupus erythematosus in humans". Nature Genetics. 32 (4): 666–9. doi:10.1038/ng1020. PMID 12402038. S2CID 20496046.
- Bennett F, Luxenberg D, Ling V, Wang IM, Marquette K, Lowe D, Khan N, Veldman G, Jacobs KA, Valge-Archer VE, Collins M, Carreno BM (January 2003). "Program death-1 engagement upon TCR activation has distinct effects on costimulation and cytokine-driven proliferation: attenuation of ICOS, IL-4, and IL-21, but not CD28, IL-7, and IL-15 responses". Journal of Immunology. 170 (2): 711–8. doi:10.4049/jimmunol.170.2.711. PMID 12517932.
- Wang S, Bajorath J, Flies DB, Dong H, Honjo T, Chen L (May 2003). "Molecular modeling and functional mapping of B7-H1 and B7-DC uncouple costimulatory function from PD-1 interaction". The Journal of Experimental Medicine. 197 (9): 1083–91. doi:10.1084/jem.20021752. PMC 2193977. PMID 12719480.
- Youngnak P, Kozono Y, Kozono H, Iwai H, Otsuki N, Jin H, Omura K, Yagita H, Pardoll DM, Chen L, Azuma M (August 2003). "Differential binding properties of B7-H1 and B7-DC to programmed death-1". Biochemical and Biophysical Research Communications. 307 (3): 672–7. doi:10.1016/S0006-291X(03)01257-9. PMID 12893276.
- Nielsen C, Hansen D, Husby S, Jacobsen BB, Lillevang ST (December 2003). "Association of a putative regulatory polymorphism in the PD-1 gene with susceptibility to type 1 diabetes". Tissue Antigens. 62 (6): 492–7. doi:10.1046/j.1399-0039.2003.00136.x. PMID 14617032.
- Prokunina L, Gunnarsson I, Sturfelt G, Truedsson L, Seligman VA, Olson JL, Seldin MF, Criswell LA, Alarcón-Riquelme ME (January 2004). "The systemic lupus erythematosus-associated PDCD1 polymorphism PD1.3A in lupus nephritis". Arthritis and Rheumatism. 50 (1): 327–8. doi:10.1002/art.11442. PMID 14730631.
- Lin SC, Yen JH, Tsai JJ, Tsai WC, Ou TT, Liu HW, Chen CJ (March 2004). "Association of a programmed death 1 gene polymorphism with the development of rheumatoid arthritis, but not systemic lupus erythematosus". Arthritis and Rheumatism. 50 (3): 770–5. doi:10.1002/art.20040. PMID 15022318.
- Prokunina L, Padyukov L, Bennet A, de Faire U, Wiman B, Prince J, Alfredsson L, Klareskog L, Alarcón-Riquelme M (June 2004). "Association of the PD-1.3A allele of the PDCD1 gene in patients with rheumatoid arthritis negative for rheumatoid factor and the shared epitope". Arthritis and Rheumatism. 50 (6): 1770–3. doi:10.1002/art.20280. PMID 15188352.
- Sanghera DK, Manzi S, Bontempo F, Nestlerode C, Kamboh MI (October 2004). "Role of an intronic polymorphism in the PDCD1 gene with the risk of sporadic systemic lupus erythematosus and the occurrence of antiphospholipid antibodies". Human Genetics. 115 (5): 393–8. doi:10.1007/s00439-004-1172-0. PMID 15322919. S2CID 8562917.
- Nielsen C, Laustrup H, Voss A, Junker P, Husby S, Lillevang ST (2005). "A putative regulatory polymorphism in PD-1 is associated with nephropathy in a population-based cohort of systemic lupus erythematosus patients". Lupus. 13 (7): 510–6. doi:10.1191/0961203303lu1052oa (inactive 2024-04-12). PMID 15352422. S2CID 33705026.
{{cite journal}}: CS1 maint: DOI inactive as of April 2024 (link) - Johansson M, Arlestig L, Möller B, Rantapää-Dahlqvist S (June 2005). "Association of a PDCD1 polymorphism with renal manifestations in systemic lupus erythematosus". Arthritis and Rheumatism. 52 (6): 1665–9. doi:10.1002/art.21058. PMID 15934088.
- Nielsen C, Ohm-Laursen L, Barington T, Husby S, Lillevang ST (June 2005). "Alternative splice variants of the human PD-1 gene". Cellular Immunology. 235 (2): 109–16. doi:10.1016/j.cellimm.2005.07.007. PMID 16171790.
- Parry RV, Chemnitz JM, Frauwirth KA, Lanfranco AR, Braunstein I, Kobayashi SV, Linsley PS, Thompson CB, Riley JL (November 2005). "CTLA-4 and PD-1 receptors inhibit T-cell activation by distinct mechanisms". Molecular and Cellular Biology. 25 (21): 9543–53. doi:10.1128/MCB.25.21.9543-9553.2005. PMC 1265804. PMID 16227604.
- Kobayashi M, Kawano S, Hatachi S, Kurimoto C, Okazaki T, Iwai Y, Honjo T, Tanaka Y, Minato N, Komori T, Maeda S, Kumagai S (November 2005). "Enhanced expression of programmed death-1 (PD-1)/PD-L1 in salivary glands of patients with Sjögren's syndrome". The Journal of Rheumatology. 32 (11): 2156–63. PMID 16265694.
External links
[edit]- PDCD1+protein,+human at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
- Overview of all the structural information available in the PDB for UniProt: Q15116 (Programmed cell death protein 1) at the PDBe-KB.
This article incorporates text from the United States National Library of Medicine, which is in the public domain.